Carenet solves the dual problems of cost and care for IVIG treatment
PATIENT CARE COORDINATION
LIFE-SUSTAINING TECHNOLOGY
FINANCIAL
SAVINGS
CareNet provides payers with real-time real-dollar visibility into each patient receiving IVIG.
Care Management
Our proprietary platform gets payers the outcomes they desire and keeps costs under control.
We improve the treatment experience by consistent supply, choice of administrative sites and guaranteed appropriate utilization.
We provide big benefits to the payees by improving patient care, managing IVIG spending and having expert physician over site.
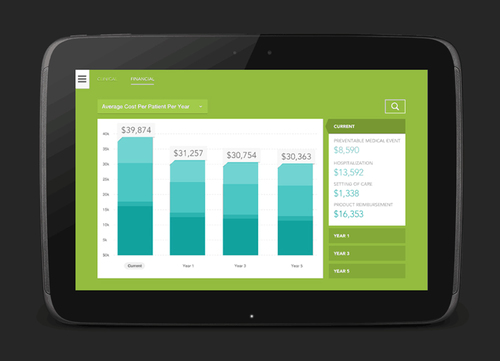
Cost Savings
CareNet significantly reduces IVIG cost for payers. The average IVIG cost per patient per year is $125,000 and CareNet 's average IVIG cost per patient per year is $75,000.
Based on a payers typical IVIG spend, CareNet believes our solution can save you millions over the next 5 years.
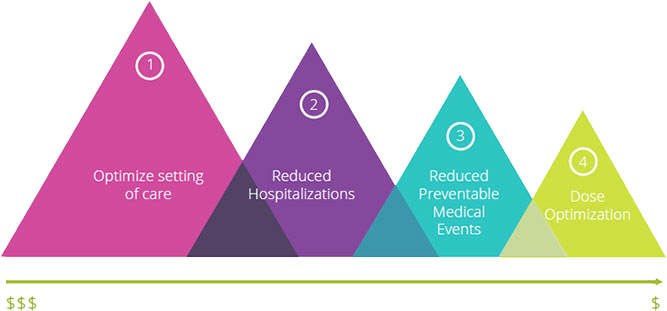
We optimize 4 levers to reduce the overall cost for payers, including: optimized setting of care, reduced hospitalizations, reduced preventable medical events, dose optimization.
How CareNet saves
We optimize 4 "levers" to reduce the overall cost for payers, including:
What does technology actually look like?
How CareNet Works
CareNet coordinates care for all of your patients receiving IVIG.
Carenet Overview
CareNet is a care coordination platform that enables health plans save money on patients requiring IVIG. The technology improves patient outcomes and lowers cost. A win-win. CareNet has been a leader in IVIG therapies for over 20 years and is widely considered an expert in autoimmune, neurologic diseases and immunologic diseases.
Most health plans don’t know how much they are spending on IVIG. This may sound shocking, but a typical health plan serving just 1,000 patients on IVIG can cost the plan over $100,000,000 per year.
The cost picture is further complicated by a few critical challenges to payers and physicians.
1.) Cost. IVIG is very expensive to procure
2.) Education. There is very little administrative education for nurses and therefore potentially preventable events
3.) Standards. It’s often dosed incorrectly, misused, and over-prescribed
However, there is good news. We believe that better treatment plus better management equals big benefits to payers. First, evidence based guidelines guarantees appropriate utilization, best site of service for the patient, and less hospitalizations. Next, better patient management means care is coordinated, non-responder patients are discontinued, and real-time data is given back to the health plan. All in, this is a big benefit to health plans.
CARENET MISSION & VALUES
Be loyal to our partners
Patient care comes first
Do the right thing
Be loyal to our physician partners
Have fun everyday
Give back

TEAM
Judi McQueary – President
Elaine Jackson, R.N. – Vice President
Jennifer McClain, R.N. – Director of Clinical Excellence
Bucky Staggs, RN, IGCN - Clinical Science Liaison
Kim Daugherty, J.D. – Corporate Compliance Officer
Lauryn Watson – Director of Creative Communications